
Three in the morning. You're awake again, drenched in sweat, your heart racing for no reason at all. You peel off your pajamas and stand in front of the open refrigerator, letting the cold air wash over you. Your partner's still sleeping. Lucky them. You wonder if this is what the rest of your life looks like now—hot flashes every twenty minutes, brain fog so thick you can't remember if you took your medication, and a constant low-level irritability that makes you snap at people you love.
Welcome to menopause. Or maybe you've already been here for months, even years, riding this wave of symptoms that nobody warned you about. Your mom didn't talk about it. Your doctor seemed rushed. Online forums are a minefield of contradicting advice and worst-case scenarios. So you're googling "menopause relief" at midnight, scrolling through ads for supplements you've never heard of, wondering what actually works and what's just marketing hype.
Here's what I want to tell you first: you're not losing your mind. You're not overreacting. And you're not alone—roughly 40% of women seek medical care for menopause symptoms, which means millions of us have sat in exactly your chair, sweating through sheets at 3 a.m., wondering what to do.
The good news? We actually have real solutions now. Not just "drink more water and do yoga." Real, evidence-based options that work. Some involve doctors and prescriptions. Some you can do at home with nothing but consistency and the right information. Some combine both. The trick is figuring out which path makes sense for your life, your body, and your situation.
What Are the Treatment Options for Menopause? Understanding Your Real Choices
When you finally schedule that doctor's appointment—and let's be honest, it takes some courage to admit you need help—you'll probably hear about "hormone replacement therapy" pretty quickly. It's the treatment that gets the most attention, mostly because it works remarkably well for a lot of people. But it's far from your only option, and it's definitely not right for everyone.
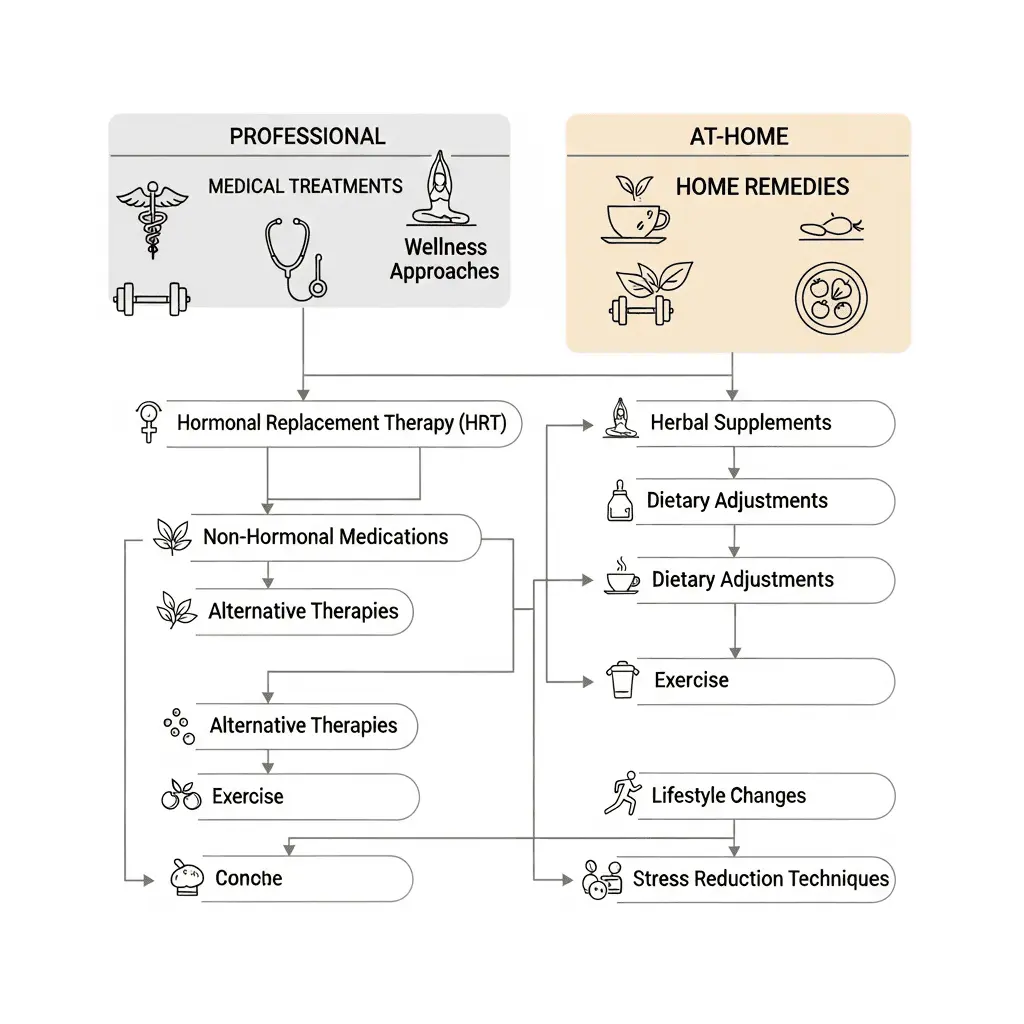
Think of menopause treatment options as falling into two main camps: what doctors can prescribe and do, and what you can manage yourself. Neither is automatically "better." Both have real advantages and real limitations. The best choice is the one that fits into your actual life.
The professional side includes prescription hormones, newer medications specifically designed for menopause symptoms, psychiatric drugs that have secondary benefits for hot flashes, and procedures that sound futuristic and actually work. The at-home side includes herbs your grandmother probably used, lifestyle changes that take time but compound over months, and structured programs you can do on your couch at midnight when the insomnia hits.
Most women end up using both. They might take a low-dose estrogen patch while also doing yoga three times a week and drinking ginger tea because, well, why not stack the deck in your favor?
Natural Treatments for Menopause That Actually Work (Not the Ones That Just Sound Good)

Let me be honest: not everything labeled "natural" works. Some of it is pure marketing. But some of it actually does help, and it's worth knowing the difference.
Black cohosh is probably the most famous herbal menopause remedy. It's been used for literally centuries. Does it work? Here's the complicated answer: some women swear by it. Some studies show it's about as effective as low-dose hormone therapy. Other studies say it's no better than placebo. The truth is probably somewhere in the middle—it helps some people, doesn't help others, and you won't know which category you're in until you try it. If you do try it, give it at least two months. These things don't work overnight.
Red clover has better research backing it than you might expect. It contains compounds that act somewhat like estrogen in your body. Eleven different studies showed it was better than placebo for hot flashes. Not dramatically better. But better. And for someone having five hot flashes a day, even cutting it down to three or four is life-changing.
Soy is interesting because it's a food, not a supplement. Women in Asian countries who eat a lot of soy report fewer hot flashes than Western women. Coincidence? Maybe. Probably not. The phytoestrogens in soy—plant compounds that mimic estrogen—seem to help. You're not going to fix menopause with tofu alone, but adding it to your diet alongside other strategies? Worth it.
Evening primrose oil doesn't work miracles, but some research suggests it can reduce hot flash severity by about 10%. That might sound small until you're experiencing it. Ten percent less severity on a 10 hot flash day means roughly one fewer hot flash and three that are slightly more bearable. People living through hot flashes do that math and say yes.
Flaxseed has lignans that some evidence suggests help balance hormones. Add it to your smoothies or yogurt. Again, not a cure-all, but part of the picture.
Sage tea sounds like a grandmother's remedy, and that's because it kind of is. Women in Europe have been drinking it for centuries. Modern research actually backs this up—one study found it reduced hot flashes by about 50% over eight weeks. Eight weeks of drinking sage tea before deciding if you notice a difference seems reasonable.
The herbs—passionflower, ginseng, dong quai, maca—all have mixed evidence. Some women in forums rave about them. The research is generally underwhelming but not zero. Think of them as worth trying if you're willing to experiment and patient enough to give them real time.
Here's the critical thing nobody tells you clearly enough: just because something is "natural" does NOT mean it's safe or effective. Some herbal supplements interact badly with medications. Some are just expensive placebo. And the placebo effect in menopause research is actually significant—women expect to feel better, so they do feel better, even when the herb isn't actually doing anything. That's not nothing from a quality-of-life perspective, but it's worth acknowledging.
Always tell your doctor what supplements you're taking. Always.
Professional Procedures for Menopausal Symptoms: When You Need Real Firepower

Some days you can't white-knuckle it through with tea and breathing exercises. Some women have hot flashes so severe and so frequent that they literally cannot function at work. Some have the kind of brain fog that makes simple tasks feel impossible. That's when professional help isn't an option—it's necessary.
Hormone Replacement Therapy
Hormone replacement therapy, despite decades of fear campaigns, remains the most effective treatment available. If you take hormones, you have about an 85% chance your hot flashes will significantly improve. For many women, they stop almost completely. The night sweats resolve. You sleep again. Your mood stabilizes. For someone who's been suffering, this is genuinely life-changing.
Here's what you need to know about HRT that your doctor probably didn't explain well: the risks are lower than you've been told. The "black box warning" that scared a generation of women? In 2025, the FDA is removing it for many formulations because newer evidence shows that for women under 60 or within 10 years of menopause, hormone therapy is actually quite safe. That doesn't mean zero risk—all medical treatments have risks—but the benefit-to-risk ratio is often heavily weighted toward benefit.
HRT comes in multiple forms. Pills. Patches. Vaginal rings. Gels. Sprays. Some work better for some women. Most women find they need to try more than one to find what doesn't give them headaches or digestive issues or other side effects. This is a normal part of finding your treatment, not a sign that HRT doesn't work for you.
Vaginal Estrogen
Vaginal estrogen is a different beast entirely. If your main problem is vaginal dryness, painful sex, or frequent urinary tract infections, you don't necessarily need systemic hormone therapy. You might just need estrogen directly in the vagina, where it can do its job without flooding your whole system with hormones. The dose is much lower than other HRT. It absorbs directly into tissue that's starving for estrogen. Many women use this alongside other treatments or alone.
New Medications Designed for Menopause
New medications are arriving that weren't available five years ago. Fezolinetant (brand name Veozah) is designed specifically for vasomotor symptoms—hot flashes and night sweats. It works differently than estrogen, targeting the part of your brain that controls temperature regulation. In clinical trials, it reduced hot flashes by more than 50% compared to placebo. For women who can't take hormones or whose symptoms don't improve with standard options, this is genuinely exciting.
Psychiatric Medications with Secondary Benefits
SSRIs and SNRIs (the antidepressants) reduce hot flashes in a surprising percentage of people. This wasn't the original purpose of these drugs, but it's a well-documented side benefit. Paroxetine at a low dose is particularly effective. If you also happen to have depression or anxiety—which often goes hand-in-hand with menopause—this is a two-for-one solution. Not as effective as estrogen, but substantial enough to matter.
Gabapentin is a nerve medication that helps with hot flashes. It's not primarily designed for menopause, but it works. Studies show it reduces hot flashes by about 54% and the overall hot flash score by 30-50%. Good enough that it's a standard recommendation, especially for women who can't take hormones.
Specialized Procedures
The stellate ganglion block is the sci-fi option. A doctor injects local anesthetic into a nerve cluster in your neck—the stellate ganglion—which is part of your sympathetic nervous system. This system controls your fight-or-flight response and, apparently, your temperature regulation. Women who get this procedure report significant hot flash reduction. Some women report relief for six months or longer after a single injection. It's invasive, it's expensive (around $2,000), and the research isn't enormous yet, but for women with severe symptoms who've tried everything else, it's an option that actually works for some people.
Cognitive behavioral therapy delivered by an actual therapist is in this professional category, though you can also do a version at home. When delivered by a professional, it involves learning specific techniques for managing how you respond to hot flashes, understanding your thought patterns about menopause, and actually rewiring your stress response. It takes time and commitment, but the results stick around even after you stop therapy. And if you're also dealing with anxiety or mood issues—again, common during menopause—CBT helps with all of it.
Treating Hot Flushes and Other Common Menopausal Symptoms: The Practical Toolkit

Hot flushes are the symptom everyone talks about, probably because they're incredibly disruptive. You're in a meeting, feeling fine, and suddenly your face is burning and you're visibly sweating. At a dinner party, the people around you wonder if something is wrong. At night, you wake up drenched, freezing, and you have to get up and change your pajamas and sheets. Again.
Pharmaceutical Approaches
If hormone therapy is available to you and works, that's your quickest path to relief—77% reduction in hot flash frequency and severity. That's not exaggeration. That's actual clinical data.
If you can't or won't take hormones, SSRIs like paroxetine at low doses reduce hot flashes by 24-69%. That's a massive range, which tells you it works really well for some people and does almost nothing for others. You won't know which until you try, but if it works, you'll notice in about a week or two.
Gabapentin is slower to work—it takes a few weeks—but it's reliable. Most women get meaningful reduction, even if not total elimination.
Venlafaxine, an SNRI, works particularly well at 75 mg doses. For women taking tamoxifen for breast cancer, this is actually the recommended drug.
Oxybutynin, which was originally designed for overactive bladder, reduces hot flashes by 70-86% in some women. Weird, but true. And if you happen to have urinary frequency issues, you've solved two problems with one medication.
None of these are perfect. All have potential side effects. But they're options, which is better than suffering through.
Complementary Therapies
Acupuncture is in this weird middle ground. Some women get real relief from it. Research shows it beats no treatment but doesn't beat sham acupuncture—meaning a lot of the benefit might be placebo. But honestly? If someone gets relief, does the mechanism matter? If you find an acupuncturist and it helps, that's a win.
Lifestyle Strategies You Can Do Right Now
- Stay cool. Keep fans in your bedroom and workspace. Wear layers you can remove. Sleep with cotton sheets, not synthetic. This sounds simple because it is simple, but it actually helps.
- Avoid triggers. Hot spicy foods, alcohol, coffee in the evening, hot beverages—all of these can trigger or worsen hot flashes for many women. You might not have triggers at all. You might have specific ones. Pay attention.
- Lose weight if you need to. Excess weight is correlated with more frequent and more severe hot flashes. Losing even 5-10% of body weight can help significantly.
- Exercise. Regular physical activity reduces hot flash frequency and severity. This is consistent across research. Why? Probably several reasons—exercise helps regulate hormones, reduces stress, improves sleep, and changes your body's thermoregulation.
- Manage stress. Stress absolutely makes hot flashes worse. Meditation, deep breathing, yoga, therapy—whatever helps you actually reduce your stress load, not just pretend to.
- Sleep properly. Night sweats wake you up, which disrupts sleep, which makes you more stressed, which makes symptoms worse. It's a cycle. Good sleep hygiene—dark room, cool temperature, no screens an hour before bed, regular schedule—matters.
At-Home & Non-Hormonal Solutions: What You Can Actually Do Right Now

Not everyone wants to see a doctor. Not everyone has access. Not everyone's insurance covers menopause treatments. Not everyone has time to wait for appointments. So what can you actually do at home, right now, that has evidence behind it?
Self-help cognitive behavioral therapy is surprisingly effective. There are workbooks, online programs, and apps designed specifically for menopausal women. They walk you through techniques for recognizing unhelpful thought patterns about your hot flashes, learning to reframe them, and developing actual coping strategies. Studies show that women who work through these programs seriously—meaning they actually do the exercises, not just read them—get significant improvements in how bothersome hot flashes feel, even if the frequency doesn't change dramatically. The improvement sticks around after you stop, too.
Exercise is genuinely the best thing you can do. At least 150 minutes per week of moderate activity. This could be brisk walking, cycling, swimming, whatever. Add in two days of strength training and balance work. Yes, this takes time. But if you're going to pick one lifestyle change to commit to, this is it. Exercise reduces hot flashes. It improves sleep. It helps with mood. It protects your heart and bones, which become more vulnerable as estrogen drops. It literally improves every measure of menopause quality-of-life.
If you hate the gym, this doesn't have to be gym-y. Walking counts. Dancing counts. Playing with your kids counts. Gardening counts. Anything that gets you moving for 30 minutes and leaves you slightly breathless.
Yoga and meditation are not magic, but they help. Specifically, they help calm your nervous system. If your hot flashes are tied to stress and anxiety—and for many women they are—regular yoga practice can genuinely reduce flashes. Even 20 minutes of yoga three times a week shows up in research. Meditation isn't about clearing your mind (that's a myth, by the way). It's about teaching yourself to notice thoughts without being swept up in them. During a hot flash, this is actually useful. You notice the hot flash starting, and instead of panicking—which makes it worse—you just observe it.
Diet changes matter more than you think. You don't need a special "menopause diet." You just need to eat actual food. Whole grains instead of refined ones. Vegetables instead of processed snacks. Protein at every meal. Good fats—olive oil, fish, avocados, nuts. Calcium from greens and dairy if you eat it. Vitamin D, which is harder to get unless you're taking a supplement.
Hot triggers are different for everyone, but spicy foods, alcohol, and caffeine frequently make symptoms worse. Try cutting them out for two weeks and see if your hot flashes improve. If they do, you know you found something. If they don't, add them back.
Sleep. This deserves its own line item. You cannot manage menopause symptoms well if you're sleep-deprived. Night sweats are stealing your sleep. Insomnia from hormonal changes is stealing your sleep. And less sleep makes every symptom worse. Invest in cooling sheets if you night sweat. Invest in a fan. Keep your bedroom cool and dark. No screens an hour before bed. Same bedtime every night. This is foundational.
Supplements like Amberen are over-the-counter options. They're not FDA-approved drugs, so the evidence is different. Some women report real improvement—reduction in hot flashes, better mood, more energy. Other women notice nothing. The research on the specific ingredients is mixed. But if you want to try something and aren't having severe symptoms, it's worth the money to experiment.
Stress management tools aren't luxuries. They're actually part of your treatment toolkit. Whatever helps you actually feel calmer—therapy, support groups, time with friends, creative pursuits, time in nature—do more of it. Your nervous system's stress level directly affects your menopause symptoms.
The beautiful thing about at-home options is you can combine them. You don't have to pick one. Exercise plus yoga plus diet change plus meditation is way more powerful than any one of those alone.
Early and Post-Menopause Care: When Menopause Happens "Too Soon"

If you're reading this and menopause started when you were in your 30s or early 40s, your situation is different. Either you're dealing with premature ovarian insufficiency (POI), or you had cancer treatment that triggered early menopause, or a hysterectomy/oophorectomy, or you have a genetic condition. Whatever the cause, early menopause isn't just about hot flashes.
Early Menopause and Health Risks
Early menopause significantly increases your risk of osteoporosis, heart disease, cognitive decline, and premature death. These aren't hypothetical risks. These are substantial, documented risks. Which means you need to take this seriously.
For women with early menopause, hormone replacement therapy is basically mandatory unless there's a serious contraindication like untreated breast cancer. You're not replacing hormones for comfort or convenience—you're doing it to prevent serious long-term health consequences. The hormone therapy needs to continue until you reach the average age of natural menopause (around 50 or 51).
This is different from treating menopause that starts naturally at 50. Different doses, different duration, different goals.
Beyond hormones, early menopause means:
- Bone density screening. Get it checked. Osteoporosis can develop rapidly when you lose estrogen young.
- Heart health attention. Regular blood pressure checks, cholesterol panels, exercise. Your cardiovascular risk profile changed.
- Fertility considerations. If you wanted biological children, you need to talk to specialists about whether anything is possible. Sometimes it is, depending on the situation.
- Mental health support. Early menopause carries emotional weight. Grieve what's happening if you need to. Get support if the adjustment is hard.
Post-Menopause (Years After Your Last Period)
After menopause—meaning you're five, ten, twenty years past your last period—the acute symptoms have resolved, but the maintenance work continues.
- Bone health stays important. If you stopped doing weight-bearing exercise, start again. Osteoporosis prevention never stops mattering.
- Heart health matters more as you age. Cholesterol, blood pressure, weight, blood sugar—all the things that matter for everyone, but especially for people without estrogen's cardiovascular protection.
- Some women have lingering symptoms even years post-menopause. Vaginal dryness can persist. Sleep issues can persist. If that's you, continuing treatment (even if just low-dose vaginal estrogen) is okay.
- The biggest thing post-menopause is making sure you don't become sedentary. Use it or lose it applies to muscles, bones, brain, and heart.
How to Choose the Right Menopause Treatment for You: A Practical Decision Guide

You're probably overwhelmed by now. All these options. How do you actually pick?
An Eight-Step Decision Process
Step one: Know your symptoms. Are hot flashes destroying your life, or are they annoying but tolerable? Do you have vaginal dryness making sex painful? Brain fog that's affecting your work? Mood changes that are scary? Insomnia? Probably you have multiple symptoms. Write them down. Rate them for severity and how much they're actually impacting your daily life. "I have one hot flash per week and barely notice" is different from "I have ten hot flashes daily and I'm considering quitting my job."
Step two: Know your health history. Do you have a personal or family history of breast cancer? Blood clots? Heart disease? Stroke? These matter for medication choice. If you have certain contraindications, some options are off the table. Some aren't. Talk to your doctor specifically about your risks.
Step three: Decide what you're comfortable with. Are you ideologically opposed to hormones? That's okay—other options exist. Are you willing to try natural approaches first and see if they help? That's reasonable. Do you want the most effective treatment even if it's a prescription? That's also fine. There's no wrong answer here as long as you're making an informed choice.
Step four: Consider logistics. How much time do you have for self-care? If you have zero time to exercise, recommending that you do 150 minutes weekly is pointless. If you can't afford $200 per month on supplements, don't go that route. Be realistic about your actual life, not your aspirational life.
Step five: Combine intelligently. Hormone therapy plus exercise plus stress management is more powerful than any one alone. Natural supplements plus diet change plus sleep hygiene might be enough for your symptoms. The combination that works is the one you'll actually stick with.
Step six: Pick a starting point and give it real time. Most treatments need at least four to eight weeks to show full effect. If you try something for two weeks and quit, you won't know if it would have worked. Conversely, if something is genuinely not working after two months, time to try something different.
Step seven: Track what's happening. Keep notes on your symptoms. Are they getting better? Worse? Staying the same? This isn't obsessive—it's useful data for you and your doctor to evaluate whether treatment is actually helping.
Step eight: Don't suffer in silence. If something isn't working, tell your doctor. If something is working but has side effects you hate, tell your doctor. Treatment adjustments are normal and expected.
Why This Matters: A Real Conversation About Quality of Life
Menopause isn't a disease that needs curing. It's a normal part of female aging. But that doesn't mean you have to suffer through it. The fact that women have been suffering through menopause for millennia doesn't mean you should too.
You deserve to sleep. You deserve to not have your work interrupted by overwhelming hot flashes. You deserve to feel like yourself. You deserve sex to not be painful. You deserve clarity of thought. You deserve mood stability.
These aren't luxuries. They're baseline quality of life. And right now, in 2025, we have real tools to help.
The medical field is finally taking menopause seriously. Menopause clinics are opening at major medical centers. Doctors are getting specialized training. Research is happening. The stigma is starting to shift. Women are talking about it instead of suffering silently.
But that only helps if you take action. If you reach out. If you say "I'm struggling and I need help."
Your Action Steps
- Schedule an appointment with a doctor. Ideally one who has training or interest in menopause. If your current doctor dismisses your symptoms, find a different one.
- Come prepared. Write down your symptoms, when they happen, how they're affecting your life. Bring this list. Don't downplay things to be polite. The more detail you give, the better care you'll get.
- Ask questions. If your doctor recommends something, ask why. Ask about alternatives. Ask about side effects. If you don't understand something, ask again.
- Be honest about what you're willing to do. If you're not going to exercise, say that. Your doctor can adjust recommendations accordingly. False commitments don't help anyone.
- Be willing to adjust. Your first treatment might not be your forever treatment. That's normal.
- Seek support. Talk to other women. Join a support group. Find your people. Menopause isn't meant to be suffered through alone.
This is your one life. Your one body. You get to decide what quality of life looks like for you and how much effort you're willing to put into achieving it. There are real solutions. There are real options. The only thing between you and feeling better is actually taking action.
The worst that happens? You try something and it doesn't work, and you try something else. The best that happens? You sleep through the night again. You stop needing to change clothes three times daily. You feel like yourself. Your relationships improve because you're not irritable all the time. Your work performance improves because you can think clearly again.
That's worth the effort.

