Understanding Dermatitis During Menopause: The Hormonal Connection
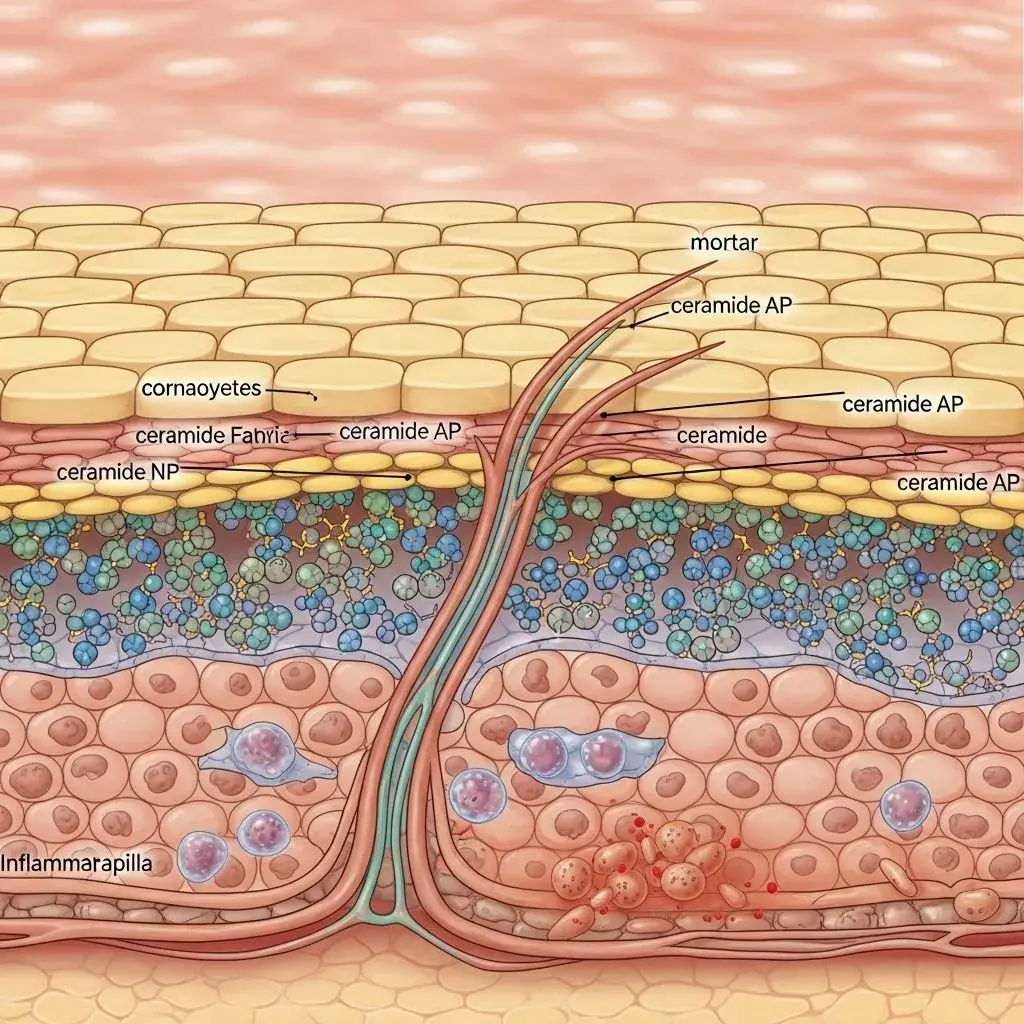
Dermatitis during menopause isn't simply aging skin—it's an inflammatory response triggered by declining estrogen levels that fundamentally alter your skin's immune function and barrier integrity. Research shows that estrogen withdrawal reduces ceramide production by 30-40%, compromising the skin barrier that normally keeps irritants out and moisture in. This creates a perfect environment for inflammatory dermatitis conditions to emerge or dramatically worsen, even in women who never had sensitive skin before.
The connection between hormones and skin inflammation involves multiple mechanisms. Estrogen regulates mast cell activity—the cells responsible for releasing histamine during allergic reactions. As estrogen drops during perimenopause and menopause, mast cells become hyperactive, triggering inflammatory responses to substances your skin previously tolerated. This explains why women suddenly develop contact dermatitis to products they've used for decades, or why atopic dermatitis that disappeared in adulthood suddenly returns with menopause.
Additionally, declining estrogen affects skin pH, shifting it from slightly acidic (protective) to more neutral or alkaline (vulnerable). This pH disruption weakens the skin's antimicrobial defenses and allows irritants to penetrate more easily, creating chronic low-grade inflammation that manifests as persistent redness, scaling, and sensitivity. Understanding these mechanisms matters because treating dermatitis during menopause requires addressing the hormonal cause, not just the surface symptoms. Learn more about hormonal skin changes in our comprehensive guide to menopausal skin care.
Common Myths vs. Evidence-Based Reality
Myth: Dermatitis Means Your Skin Is Too Dry
Many women assume menopausal dermatitis is simply dryness requiring heavier moisturizers, but true dermatitis is an inflammatory immune response, not just dehydration. Piling on rich creams can actually worsen certain dermatitis types by trapping inflammation or feeding malassezia yeast in seborrheic dermatitis cases. The misconception leads to months of ineffective treatment while inflammation persists and potentially spreads.
What actually works: identifying the specific dermatitis type first. Atopic dermatitis responds to ceramide-rich barrier repair, contact dermatitis requires elimination of triggers, and seborrheic dermatitis needs antifungal ingredients. The treatment approach differs dramatically based on type, yet all present with similar redness and flaking initially. If basic moisturizing doesn't resolve symptoms within two weeks, you're likely dealing with true inflammatory dermatitis requiring targeted treatment, not just dry skin.
Myth: Hormonal Dermatitis Only Affects the Face
While facial dermatitis gets the most attention, menopausal hormonal changes trigger body-wide inflammation patterns. Women frequently develop dermatitis on the scalp (seborrheic), hands (contact or dyshidrotic), and trunk (nummular dermatitis) during perimenopause. These body locations actually provide diagnostic clues—scalp and face involvement suggests seborrheic dermatitis, while symmetric patterns on arms and legs indicate atopic or nummular types.
The contradiction: facial treatments are marketed heavily, but body dermatitis often causes more discomfort and requires different formulations. Hand dermatitis during menopause becomes particularly problematic because hands undergo frequent washing that strips the already compromised barrier. This creates a vicious cycle where treatment must address both inflammation and constant re-injury from daily activities, requiring more intensive barrier protection than facial dermatitis.
Practical Treatment Strategies and When Standard Approaches Fail
The Elimination and Rebuild Protocol
Successful dermatitis management during menopause requires first reducing inflammation, then rebuilding barrier function—attempting both simultaneously often fails. Start with a 7-day elimination phase: use only gentle cleansers (no sulfates), skip all actives (retinoids, acids, vitamin C), and apply simple barrier repair moisturizers containing ceramides, cholesterol, and fatty acids in a 3:1:1 ratio. This mimics skin's natural lipid composition and allows inflammation to calm without new triggers.
During elimination, watch for improvement patterns. If redness and itching reduce within 3-5 days, you likely have contact or irritant dermatitis from products you're now avoiding. If symptoms persist unchanged, you may have atopic or seborrheic dermatitis requiring prescription treatment. For persistent cases, add colloidal oatmeal compresses twice daily—oatmeal contains avenanthramides that reduce inflammation through direct anti-cytokine effects, providing relief while you wait for barrier repair to take effect.
When Barrier Repair Alone Isn't Enough: The HRT Consideration
Here's the edge case most content avoids: some menopausal dermatitis cases don't respond adequately to topical treatment because the underlying hormonal deficit is too severe. Women with early menopause, surgical menopause, or particularly dramatic estrogen drops may find that topical steroids and barrier repair provide only temporary relief. The dermatitis returns within days of stopping treatment because the hormonal environment continues driving inflammation.
For these cases, hormone replacement therapy (HRT) or topical estrogen may be necessary to control dermatitis, not just for other menopause symptoms. Studies show that estrogen therapy reduces inflammatory markers in the skin and restores ceramide production, addressing the root cause rather than managing symptoms. This is a medical decision requiring dermatologist and gynecologist consultation, but it represents an honest limitation: topical skincare has a ceiling of effectiveness when systemic hormonal changes are severe. Compare this to conditions like rosacea during perimenopause, which also responds to hormonal intervention in resistant cases.
The Trade-Off: Aggressive Treatment vs. Skin Sensitivity
Topical corticosteroids quickly control dermatitis inflammation but create dependency if used long-term—the skin becomes thinner and more reactive, requiring stronger steroids for the same effect. This is the central trade-off in menopausal dermatitis management: you can aggressively suppress inflammation with steroids and get fast relief, or you can use gentle barrier repair that takes 4-8 weeks but builds long-term skin resilience. Most women need a combination approach—short-term steroids to break the inflammation cycle, then transition to maintenance with barrier repair and trigger avoidance.
What beginners misunderstand: thinking they must choose one approach permanently. The strategic use of steroids during flares, followed by strict barrier maintenance during calm periods, provides better long-term outcomes than either extreme. The downside is complexity—you must learn to recognize early flare signs and adjust treatment proactively rather than waiting for full-blown dermatitis. This requires more skin awareness and treatment adjustment than pre-menopausal skin ever demanded.

