Understanding Oily Skin During Menopause: The Androgen Paradox
The expectation that menopause causes universally dry skin is one of the most pervasive misconceptions in women's health. While estrogen decline does reduce overall sebum production in most women, approximately 20-30% of menopausal women experience paradoxically oily skin, particularly during perimenopause. This happens because testosterone levels remain relatively stable or decline more slowly than estrogen, creating a temporary androgen dominance that stimulates sebaceous glands—the same mechanism behind teenage acne, now returning decades later.
The situation becomes more complex during perimenopause when hormone fluctuations are erratic rather than linear. You might experience bone-dry skin one week, then wake up with an oily T-zone the next, reflecting wild swings in estrogen-to-androgen ratios. This unpredictability frustrates women who bought expensive anti-aging products for dry mature skin, only to develop clogged pores and shine. The oiliness isn't imagination—studies measuring sebum production show some perimenopausal women produce as much oil as women in their twenties, completely contradicting the dry skin narrative.
Additionally, stress-induced cortisol spikes during menopause can independently trigger sebum overproduction. Cortisol stimulates the same sebaceous glands that androgens activate, creating a cumulative effect. Women experiencing significant stress alongside hormonal changes often report the greasiest skin of their entire adult lives, with makeup sliding off within hours despite using mattifying products. Understanding this helps explain why managing oily menopausal skin requires different strategies than managing teenage oiliness—the underlying hormonal pattern is distinct. Learn more about these changes in our complete guide to hormonal skin changes.
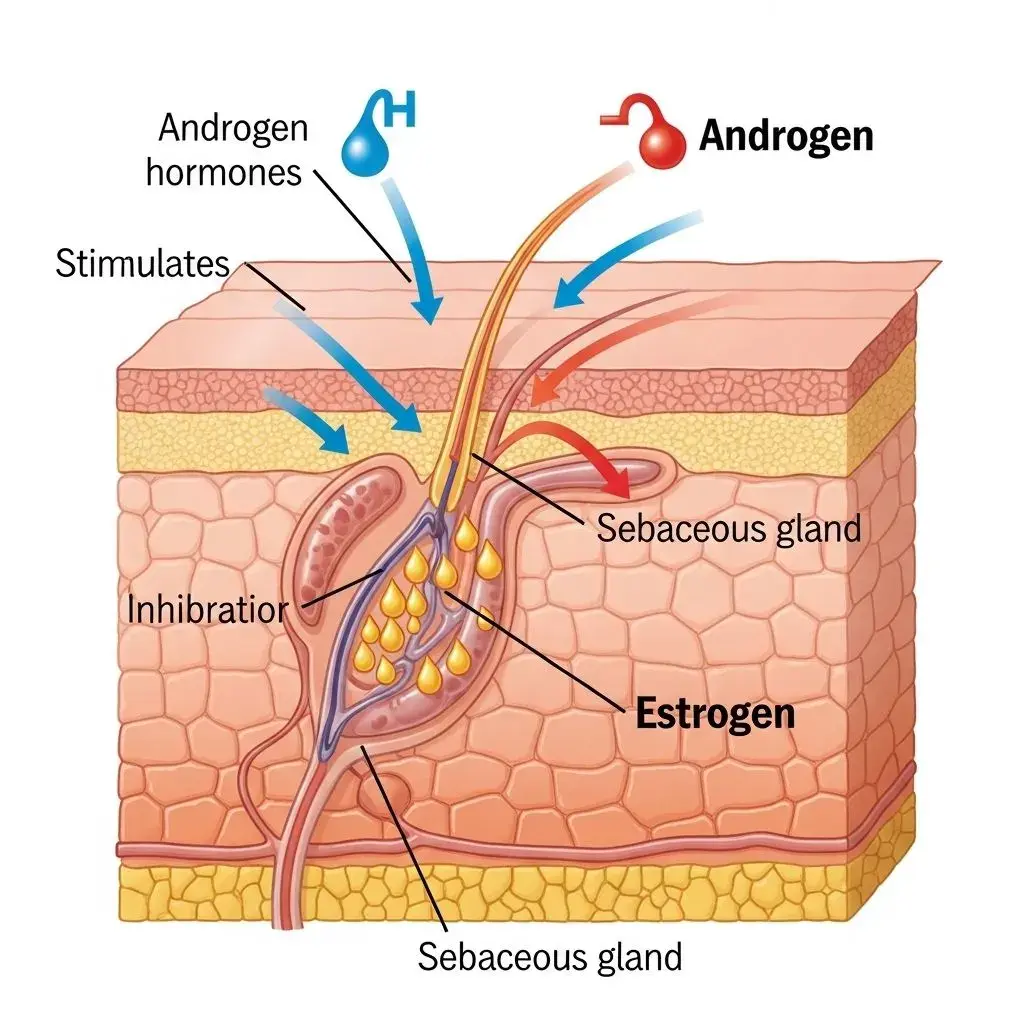
Common Myths vs. What Actually Controls Menopausal Oil Production
Myth: Harsh Cleansing Will Control the Oil
The instinct to strip oil with aggressive cleansers backfires catastrophically on menopausal skin. Unlike teenage skin that recovers quickly from stripping, menopausal skin has compromised barrier function even when producing excess oil. Harsh cleansing damages the already-vulnerable barrier, triggering reactive sebum production as skin attempts to repair itself. You end up oilier within hours, creating a cycle where more washing causes more oil.
What works instead: gentle cleansing that removes oil without destroying the barrier, followed by lightweight hydration. The contradiction is that oily menopausal skin still needs moisturizer—skipping it signals dehydration to sebaceous glands, paradoxically increasing oil production. Use gel-based or hyaluronic acid moisturizers that hydrate without adding surface oils. This balanced approach reduces oil production within 2-3 weeks as skin recognizes adequate hydration and stops overproducing sebum defensively.
Myth: Oily Skin Doesn't Need Anti-Aging Ingredients
Many women with greasy menopausal skin avoid retinoids and peptides, assuming these rich anti-aging treatments will make oiliness worse. This misconception costs years of collagen-building benefits. The reality: retinoids actually regulate sebaceous gland activity while stimulating collagen, making them ideal for oily menopausal skin. They address both the unwanted oil and the aging concerns simultaneously.
The key is choosing appropriate formulations—gel-based retinoids rather than cream-based, and starting with lower concentrations to avoid irritation that could trigger reactive oil production. Similarly, niacinamide serums reduce sebum production by up to 30% while improving barrier function and reducing inflammation. This is fundamentally different from teenage acne treatment because you're simultaneously addressing oil control and aging prevention, requiring ingredients that multitask rather than single-purpose acne actives.
Practical Management and When Standard Oil-Control Fails
The Strategic Layering System for Combination Menopausal Skin
Oily menopausal skin rarely presents uniformly—most women have an oily T-zone with dry or normal cheeks, requiring zone-specific treatment. After cleansing, apply niacinamide serum across the entire face for its barrier-supporting and sebum-regulating properties. Then split your routine: use gel moisturizer on oily zones (forehead, nose, chin) and richer cream on dry areas (cheeks, around eyes). This zone-targeting prevents the compromise of using one product that's too heavy for oily areas or too light for dry zones.
For daytime oil control, use mattifying sunscreen only on the T-zone while applying hydrating sunscreen elsewhere. Blotting papers throughout the day remove surface oil without triggering the stripping response that washing causes. At night, apply retinoid to the entire face for anti-aging benefits and sebum regulation. This strategic approach acknowledges that menopausal skin presents multiple challenges simultaneously—you can't treat it as simply oily or simply aging, requiring customization that takes more thought than pre-menopausal routines.
When Topical Treatment Isn't Enough: Hormonal Root Causes
Here's the limitation standard skincare advice avoids: severe or persistent oily skin during menopause may indicate androgen excess requiring medical evaluation, not just better products. Conditions like PCOS don't disappear with menopause and can worsen during the transition when estrogen's balancing effect diminishes. Women producing excessive androgens may develop not just oily skin but also adult acne, facial hair growth, and scalp hair thinning—a cluster suggesting hormonal intervention rather than topical treatment.
For these cases, anti-androgen medications like spironolactone or hormonal treatments may be necessary to control oil production at its source. This represents an honest edge case where topical skincare reaches its effectiveness ceiling. If you're using appropriate products correctly for 8-12 weeks without improvement, or if oily skin comes with other androgen excess signs, consult an endocrinologist or gynecologist. Compare this to other hormone-driven conditions like rosacea during perimenopause, where systemic factors require medical rather than purely cosmetic intervention.
The Trade-Off: Oil Control vs. Accelerated Aging
Aggressive oil control through drying products, frequent washing, or extremely low-fat routines will reduce shine but accelerate visible aging by damaging the skin barrier. This is the central trade-off for greasy menopausal skin: you can achieve perfectly matte skin but pay with increased wrinkles, sensitivity, and barrier damage, or you can accept some shine while maintaining skin health and slower aging. Most dermatologists recommend the middle path—moderate oil control that keeps skin comfortable without compromising barrier function.
What beginners misunderstand: believing they can achieve teenage-skin matteness while maintaining mature skin health. The reality is that some shine is acceptable and healthier long-term than over-stripping. Using blotting papers 2-3 times daily manages visible oil without the cumulative damage of constant washing or harsh products. This represents a mindset shift—accepting that oily menopausal skin is manageable but not perfectly controllable through topicals alone, especially when hormonal factors remain active.

